Hi, New Momma! Are you thinking about breastfeeding? In this blog, you’ll find a combination of information, tips, and advice to help you decide!
Firstly, we want to say that a fed baby is the best baby! Sometimes breastfeeding doesn’t work out the way you thought it would and that is completely okay! I know you may feel defeated if that happens, but remember, as long as their belly is full you’re doing it right!
Let’s talk about some of the benefits to feeding your new baby breast milk:
Nutrients
As your baby grows, your breast milk will change to meet your baby’s nutritional needs. Breastfeeding can help protect babies against some short- and long-term illnesses and diseases.
Breastfed babies have a lower risk of asthma, obesity, type 1 diabetes, and sudden infant death syndrome (SIDS). Breastfed babies are also less likely to have ear infections and stomach bugs. Breast milk shares antibodies from you to your baby. These antibodies help babies develop a strong immune system and protect them from illnesses.
Breastfeeding can reduce your risk of breast and ovarian cancer, type 2 diabetes, and high blood pressure.
Convenience
You can feed your babies on the go without worrying about having to mix formula or prepare bottles. When traveling, breastfeeding can also provide a source of comfort for babies whose normal routine is disrupted.
(Center for Disease Control 2021)
Bonding
Physical contact is very important for your baby. It helps your baby feel safe, warm, secure, and loved. The skin to skin contact from breastfeeding also boosts your levels of oxytocin, a hormone that helps breast milk flow and helps you feel calm.
Digestion
Babies can easily digest breast milk. And colostrum, the thick milk moms make during pregnancy and just after birth, helps your baby's digestive system grow.
Cost
Breast milk is free. Breastfed babies may also be sick less often, which may keep your health costs low.
(WIC Breastfeeding 2023)
Now that we’ve gone over some benefits of breastfeeding, let’s talk about what to expect if you start to breastfeed:
Remember that every mother’s experience with breastfeeding is different. Whether this is your first baby or you have many, each baby is unique. Breastfeeding will be a learning process.
Your baby is learning how to:
- Latch.
- Suck.
- Swallow.
You are learning how to:
- Position your baby to feed.
- Observe and follow his or her hunger cues (keep reading to learn more about hunger cues)
- Manage your breast milk supply and breast health.
Milk Coming In
At birth, your breasts will make a thick, yellowish substance called colostrum. Colostrum is packed with nutrients and other important substances that help your baby start building up his or her immune system. There will not be a lot of this liquid at first, but the amount will gradually increase over the first couple of days. Most babies will get all the nutrition they need through colostrum during the first few days of life. As you begin breastfeeding, your baby’s sucking will tell your body to start making milk. For most mothers, this thinner, whiter form of milk comes in by about 3 days after birth, but may take longer for first-time moms. You may notice your breasts feeling full, hard, and warm as this happens. Your baby may begin to want to breastfeed more frequently around this time.
Leaking
Your breasts may feel full and leak. Over time, the leaking may slow down as your body gets used to breastfeeding. If your breasts leak, you may find it helpful to put disposable or cloth pads in your bra.
Engorgement
Over the first few weeks after birth, your breasts may become larger, firm, warm, and uncomfortable as your body adjusts to making milk. This is called engorgement. As your breasts get used to filling and emptying as you feed your baby, this should improve. Feeding your baby frequently should help to prevent severe engorgement and relieve discomfort.
Sore Nipples
During the first few weeks of breastfeeding, your nipples may be sore or sensitive as they adjust to your baby’s sucking.
Try out our Boob-eez Nipple Covers that are easy to put on and remove to avoid wearing any tight bras!
Pain While Breastfeeding
Although your breasts and nipples may be tender or uncomfortable, once your baby is well-latched, breastfeeding should not be painful. Sometimes pain can happen if you have an improper latch, a milk duct that is clogged with milk (plugged milk duct), a breast infection (mastitis), or other issues. If you have pain while breastfeeding, especially with a fever, talk with your doctor or nurse to figure out why.
(Center for Disease Control 2021)
What is a clogged milk duct?
A clogged milk duct is when breast milk can’t flow through your breasts to your nipple because the duct transporting the milk is blocked or plugged. It causes a painful lump. You can treat a clogged milk duct at home.
How do I know I have a clogged milk duct?
One of the biggest signs of a blocked milk duct is a hard lump on your breast. It’ll be painful or sore when you touch it. It may be red or large enough to be visible if you look at your breast in a mirror. If you’ve ever dealt with engorgement, the lump from a clogged duct feels like that.
Other symptoms of a clogged milk duct are:
- Pain during letdown (letdown is the initial flow of milk).
- Pain or swelling near the lump (not your whole breast).
- The lump moves or gets smaller after pumping or feeding.
- Discomfort that subsides after pumping or feeding.
What to do if you have a clogged milk duct:
Most people can unclog a milk duct at home within two days. Continue to breastfeed (chestfeed) or pump as much as your baby needs. Don’t feed or pump more than usual as this can put more stress on the ducts and cause even more inflammation.
Some of the best ways to clear a clogged milk duct are easily remembered by the acronym B.A.I.T:
-
Breast rest: Don’t over massage or overfeed. Decrease production if you have an oversupply.
-
Advil: 800 milligrams (mg) every eight hours for 48 hours.
-
Ice: Apply for 10 minutes at a time while laying on your back. Repeat every 30 minutes.
-
Tylenol: 1,000 mg every 8 eight hours for 48 hours.
(Cleveland Clinic 2022)
Try out our Ouch Pouches that can be set in the freezer for cooling relief!
Postpartum Depression
Postpartum Depression is depression that some women feel after having a baby. Feelings of postpartum depression are more intense and last longer than those of “baby blues,” a term used to describe the worry, sadness, and tiredness many women experience after having a baby. “Baby blues” symptoms typically resolve on their own within a few days. Postpartum depression is common and doesn’t feel the same for everyone. How often symptoms occur, how long they last, and how intense they may feel can be different for each person. Mothers with postpartum depression can usually continue to breastfeed. If you think you may be experiencing postpartum depression, or have other mental health concerns, contact your healthcare provider for help right away. Many medications do pass into breastmilk, but you can work with your healthcare provider to identify treatment options that are safe to use while breastfeeding.
How to hold your baby while nursing:
The Cradle Hold

This is the first hold many mothers will try, often soon after their babies are born. To start, cradle your baby's head in the crook of your arm with your baby's nose opposite your nipple. Use that hand to support your baby's bottom. Turn your baby on his or her side, so that your baby is belly to belly to you. Then, raise your baby to your breast. You can support your breast with your other hand.
The Cross-Cradle or Crossover Hold

This hold is similar to the cradle hold, but your arms are positioned differently. Instead of supporting your baby's head in the crook of your arm, use the hand of that arm to support your breast. Your opposite arm should come around the back of your baby. Support your baby's head, neck, and shoulder by placing your hand at the base of your baby's head with your thumb and index finger at your baby's ear level. Like the cradle hold, your baby will be belly to belly to you. You may need to use a pillow on your lap to raise your baby to nipple level.
The cross-cradle position allows you to have more control over how your baby latches on (takes the breast into his or her mouth). Many moms find that they're able to get their babies latched on more deeply with this hold.
The Side-Lying Position
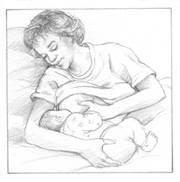
This position is comfortable for mothers who've had a cesarean section (C-section) because the baby doesn't put pressure on the mother's abdomen. Make sure that you return your baby to the crib or bassinet before falling asleep.
Start by lying on your side with your baby on his or her side, facing you. Your baby should be positioned so his or her nose is opposite your nipple. Use your lower arm to cradle your baby's back, or you can tuck a rolled-up receiving blanket behind your baby to help nestle your little one close to you while you use your arm to support your own head. You can support your breast with your other hand.
The Clutch or Football Hold

This is also a good position for the mom who's had a C-section and also for mothers with large breasts or small babies. Mothers with twins who want to feed the babies at the same time may also choose this position.
To achieve the clutch (or football) hold, place a pillow next to you. Cradle your baby — facing upward — in your arm. Use the palm of your hand on that same arm to support his or her neck, and nestle your baby's side closely against your side. Your baby's feet and legs should be tucked under your arm. Then lift your baby to your breast.
(Kids Health 2018)
Common Questions About Breastfeeding
How do I know if I'm producing enough milk?
Most moms will make enough breast milk with no problems. To make sure, you should monitor your baby's wet and soiled diapers. Babies who get enough to eat will go through five to six diapers a day once your milk fully comes in. Also, your pediatrician will check your baby's weight regularly.
How do I know I'm doing it right?
They’ve found that moms just need reassurance. You can ask your health care provider or consult with a breastfeeding specialist or public health nurse. These specialists can check that you and baby are positioned comfortably and assess the latch on the breast. They also can answer any questions. Learning to breastfeed can feel overwhelming in the beginning, but we're fortunate to have so many resources who are here to help you set and reach the goals best for you and your baby.
How will I know when my baby is hungry?
Newborns need to eat at least eight to 12 times during a 24-hour period. Watch your baby, not the clock. Babies give cues when they're hungry. These include rooting from side to side, putting their hands up to their mouth, and searching for a breast or nipple. You'll quickly learn to recognize these cues. Crying is the last sign of hunger, so it's important to try to feed before crying starts. It can be difficult to calm a crying baby and get them latched.
(Mayo Clinic Health System 2021)
What are the crucial rules for breast milk storage?
4/4/6-12 rule
The 4/4/6-12 rule states that you can safely store your breastmilk for about 4 hours at room temperature, 4 days in the fridge, and 6-12 months in the freezer. So to break things down further: If you know you will be using your breastmilk at the next feeding, just keep it on your counter! If you know you won’t be needing your freshly pumping breastmilk in the next 5 days, then put it straight into your freezer.
Include the date it was pumped
Get into the habit of writing the date that you pumped that breast milk onto its storage container. This will allow you to use up the oldest milk first to minimize waste.
Store it flat, for storage sake, in containers of 2-5 oz
Did you know that babies from 1-6 months old take in the same amount of breastmilk? That amount is about 2-5 ounces per feed. Based on that, try and store your breastmilk in containers no larger than 2-5 ounces. That will make it easy to thaw out one feeding at a time. Once the milk is thawed, it needs to be used within 24 hours, so smartly stored amounts will ensure less wasted milk.
How do I thaw and warm up breast milk?
Plan Ahead
It’s best to thaw milk in the fridge, so plan when possible. For example, if you are going to work the next day, pull out the breast milk that you will be taking to your caregiver the night before. Try and use your oldest dated milk first. Think first in, first out. Thawed milk should be used within 24 hours, so plan accordingly.
Avoid microwaves
Warming milk in the microwave can break down the good nutrients and also create hot spots. Instead, warm it up by running the container under warm water or setting it in a bowl of warm water. You can also consider purchasing a bottle warmer, especially if you are planning to thaw large amounts at a time. Did you know that you can feed your baby breast milk straight from the fridge? It can even be at room temperature. Just know that it may take some getting used to from your baby since it’s not the same temperature as when it comes straight from your breast.
Test the milk on your wrist
After you’ve thawed and prepared your baby’s breastmilk, be sure to always check the temperature on your wrist before feeding it to your baby. Swirl the milk to mix in fat that may have separated, and Bon Appetit to your baby!
(Love Majka 2021)
What if breastfeeding isn’t right for you?
As a new parent, it can be frustrating and upsetting to realize that your plan to breastfeed your little one isn't a viable option anymore. Sometimes, for reasons such as engorgement, latch issues, or nipple soreness, breastfeeding does not work despite your—and your baby's—best efforts. It’s natural to feel a deep disappointment and sense of failure at not being able to feed baby at your breast. Breastfeeding isn't an option for everyone.
Know the Facts
The truth is that breastfeeding doesn't work for everyone. Some 60 percent of mothers don't end up breastfeeding for as long as they intended to, according to the Centers for Disease Control and Prevention. You are not alone in this experience and it's not a reflection on you as a parent or person. Also, not breastfeeding doesn't mean your baby won't be healthy or well-fed. Formula is a very healthy alternative to breast milk and your baby will be just as happy, loved, and nourished as a breastfed baby.
Remember that Fed Is Best
It's important to know that formula-fed babies can and do thrive. It is well-established that breast milk is the optimal form of nutrition for babies; however, the American Academy of Pediatrics acknowledges that this is not always possible, and moreover, they agree that "fed is best." Research also makes clear that if breastfeeding does not work for you and your baby, formula is a sound alternative and provides all the nutrition your baby needs to grow and develop.
Embrace the Positives
While breastfeeding has its own health benefits, formula feeding offers distinct advantages, too. First and foremost, formula-fed infants tend to sleep longer and better, and they don't have to feed quite so often. More than likely, this means you will be getting more sleep, sooner, too. Additionally, bottle feeding can be done by anyone, not just the person who delivered the baby. So, this job can be shared among partners or taken on by family, friends, or caregivers.
Grieve the Loss of Not Being Able to Breastfeed
If you're feeling sad about not being able to breastfeed, acknowledge and express your feelings. Let yourself feel frustrated, disappointed, or mad. Share your grief with trusted family members, friends, your healthcare provider, or a therapist. Letting out your feelings can be the first step in moving on and making peace with the situation. Once you've given yourself a chance to be sad, you'll be better equipped to let that disappointment go as you shift to focusing on your baby.
Get Help if Needed
If you feel you are having trouble processing your grief or it is keeping you from your daily activities, seek out help. A therapist or your healthcare provider can offer guidance and support. New parents are at risk of postpartum depression as we’ve talked about above, so be sure to consider if your sadness has become something that needs professional attention.
Signs to watch out for include mood swings, fatigue, trouble concentrating, crying spells, hopelessness, anger, despair, and anxiety.
Other Ways to Bond With Your Baby
While breastfeeding is one way to connect with your baby, it is not the only way to nurture the intimate and loving bond between parent and baby.
Feeding
Bottle feeding can be a special time with your baby. While feeding them, you can sing or talk to your child, or simply take in the wonder that is your sweet newborn. Just by giving your baby your attention, you are strengthening your bond. You still get the same time with them when bottle-feeding, and you can tell that they feel love. Their eyes say everything.
Tending to Their Needs
You can turn any time you are taking care of or cleaning up your baby into a time to connect. Bath fine, brushing their few hairs, getting them dressed, putting on lotion, or even changing their diaper, can be great occasions for bonding with your baby. Again, take the time to laugh, sing, or chat with your baby. Look them in the eye, smile at them, and stroke their cheeks or their toes. Whatever feels natural and loving to you is sure to resonate with your child.
Baby-Wearing
Wearing your baby in a sling, wrap, or baby carrier is another great way to keep them close. They will enjoy the warmth of being next to your body, the comfort of hearing your heartbeat, and spending lots of time with you.
Holding
Likewise, you can also simply hold your baby. Nothing is sweeter than cuddling up with your baby, and babies love to snuggle. Whether you are seated, standing, or lying down, you and your baby will both enjoy the experience.
Skin-to-Skin
You can also do skin to skin care. It helps boost brain development and helps regulate the baby’s blood sugar levels, heart rate, breathing, and body temperature. Holding your baby close, particularly skin-to-skin, also releases oxytocin, the “feel-good” hormone. This helps promote bonding and brain development.”
Playing
Even though a newborn can't exactly play with you, that doesn't mean you can't ply with them. You can tickle their toes, gently whisper in their ears, put your finger to their nose, give them a massage, play peek-a-boo, or lightly blow air on their face. You can get down on the ground with them during tummy-time and read them books or demonstrate fun, age-approriate toys. The possibilities are endless and sure to bring lots of joy for you both.
(Very Well Family 2022)
Disclaimer: Bean to Sprout are not experts on this subject. All articles have been cited to the original authors underneath each paragraphs.

